Introduction
Wound exudate is a normal part of the healing process, however, exudate can have both positive and negative effects on the wound (Gibson et al, 2009). Too little exudate may result in wounds drying out and therefore extend the healing process, while too much exudate can lead to problems such as maceration and prolonged inflammation, providing an ideal environment for bacteria to proliferate (Moore and Strapp, 2015).
Many patients have long-term wounds that arise as a result of underlying pathology such as venous insufficiency, diabetes, cardiovascular problems and mobility issues (Guest et al, 2016). These long-term conditions can also lead to delayed healing, putting the wound at an increased risk of infection, and biofilm development. In turn, the wound may produce an excessive volume of exudate which, if poorly managed, can lead to maceration of the surrounding skin. Figure 1 shows the effect of wound exudate if allowed to leak onto the surrounding skin.
In clinical practice, gelling fibre dressings are often used to manage highly exuding wounds in part due to their ability to absorb and retain exudate. They may also be used with absorbent secondary dressings which can help when managing a large volume of exudate. Gelling fibres are also commonly used to manage cavity wounds.
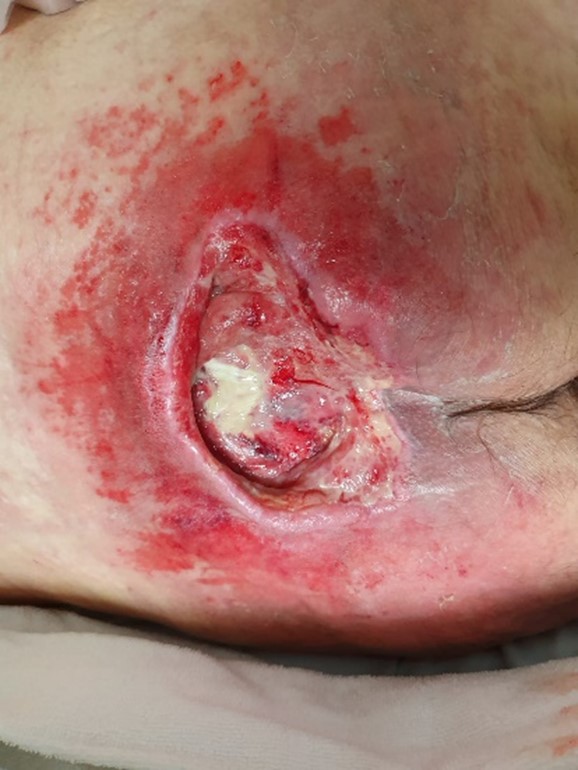
Figure 1. A patient with a Category 3 pressure ulcer and damage to the surrounding skin caused by excessive exudate.
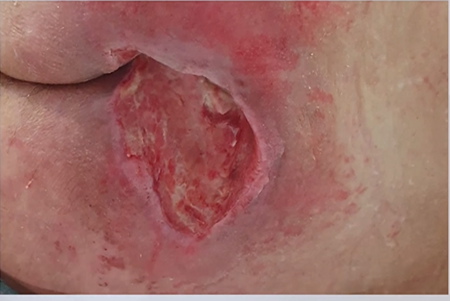
Figure 2. The same patient following 1 week of Exufiber Ag+ and Mepilex Border Sacrum Dressings (acknowledgement: Paolo Alves, Portugal, for supplying images)
New range of gelling fibre dressings with PVA fibre technology
A new range of gelling fibre dressings using polyvinyl alcohol (PVA) fibre technology has recently been developed. These polyvinyl alcohol fibres are more tightly packed than carboxymethylcellulose (CMC) fibres found in other gelling fibre products. This leads to fewer gaps in the dressing, which allows wound exudate to travel into the dressing not only to be absorbed but also to allow fluid to transfer to the secondary dressing. The tightly packed fibres also allow extra absorbency and create a dressing with a strong tensile wet strength. This helps the dressing to be removed in one piece and avoid breaking up in the wound.
Exufiber is the standard gelling fibre dressing which would be used when there is no infection or no risk of infection and Exufiber Ag+ contains silver sulphate ions which should be used to manage wounds which are infected, critically colonised or may contain biofilm. Important features of gelling fibre dressings include the ability to form a soft conformable gel on the wound bed in order to provide moist wound healing. This feature also promotes autolytic debridement for wounds with slough present. Gelling fibres are also highly absorbent and will retain this moisture even when under compression, an important feature when being used to manage patients with venous disease under compression therapy. Another key feature is the conformability of the products. This allows the gelling fibre to maintain good contact with the wound bed, aiding absorption and preventing the pooling of fluid. Exufiber and Exufiber Ag+ have been shown to facilitate the transfer of exudate to a secondary dressing, thus again preventing the pooling of fluid and reducing the risk of infection and maceration of the surrounding skin (Lustig and Gefen, 2022).
Gelling fibre dressings are available in ribbon form making them easy to insert into cavity wounds and helping to establish contact with the cavity base and walls, supporting the healing process and absorbing wound exudate. The one piece removal minimising the risk of fibre shed within the wound.
Figure 1 demonstrates poorly managed exudate in a patient with a large sacral pressure ulcer resulting in maceration and irritation of the surrounding skin. The wound was later managed with Exufiber Ag+ (primary dressing) and Mepilex Border Sacrum, silicon foam dressing (secondary dressing), and after one week of treatment, there was a significant improvement in the condition of the surrounding skin (Figure 2).
In order to gauge the clinical impact and clinician satisfaction with the Exufiber product range, a survey of 300 clinicians across 12 countries was carried out. The response rate for the survey was 87%.
Method
This survey was set up in order to gather general post market feedback on the use of Exufiber and Exufiber Ag+, such as, which wound types were most suitable, what were the benefits of using the products and would there be any situations where Exufiber would not be suitable.
The survey (Figure 3) was designed to obtain real world experiences of clinicians using the dressings in everyday clinical practice. Most of the sites already used both Exufiber and Exufiber Ag+, however, where this was not the case, sites were supplied with dressings for evaluation. 340 clinicians were approached, and 300 clinicians responded to the survey.
The survey was conducted in both paper based and electronic forms, taking only 5–7 minutes to complete. There were 15 multiple choice and free text questions enquiring about all aspects of the dressing performance, including, exudate retention under compression therapy, ability for one piece removal, prevention of maceration, overall absorbency, exudate management and ability of the product to promote autolytic debridement. The questionnaires were distributed either via email or through local clinical representatives. Both new customers and established customers were included in the survey.
Results
A total of 300 completed surveys were submitted from 23 countries worldwide (table 1). Countries included in the survey were selected where the products were already being marketed.
Of the patients reported in the survey a variety of wound types/aetiologies were included, such as venous leg ulcers (n=123), other leg ulcers (n= 31), diabetic foot ulcers (n=61), foot ulcers (not diabetes related) (n=4), other wound types (these included traumatic wounds, skin tears, haematoma) (n=44), pressure ulcers (n=21), surgical wounds (n=15) and malignant wounds (n=1) (Figure 4).
The majority of clinicians reported on their use of Exufiber Ag+ (n=236) with 64 clinicians submitting a review of the standard Exufiber product. In order to better understand the split of results, these are presented in figure 5.
Both the standard gelling fibre dressing and the silver containing version scored highly among clinicians for one piece removal the results are listed below.
Table 1. Countries included in the survey
Bulgaria
Czech Republic
Croatia
Hungary
Greece
Italy
Portugal
Serbia
Slovakia
Slovenia
Spain
United Kingdom
United States
Bulgaria
Czech Republic
Croatia
Hungary
Greece
Italy
Portugal
Serbia
Slovakia
Slovenia
Spain
United Kingdom
United States
Figure 3 The survey
Wound types (select all that apply)
Leg ulcers Foot Ulcer Abrasion Skin Tear Blister Traumatic wound Surgical wound Burns Pressure Ulcers
Wound locations
Enter your answer
Use of other interventions such as compression/off-loading (please specify)
Enter your answer
Please list the name(s) of other dressings used
Enter your answer
Clinical reason for using the product
Enter your answer
Clinical reasons for choosing dressing regime
Enter your answer
Size of dressing used
Enter your answer
Please comment on the performance of Exufiber/Exufiber Ag+
Very Good
Good
Adequate
Poor
Ease of handling
Ease/speed of application/use
Consistency of product
Ability to be repositioned during application
Conformability
Patient comfort during wear
Ability to absorb exudate
Ability to retain exudate
Performance when used under compression
Ability to maintain integrity during wear time and on removal
Ease/speed of removal
Ability to be removed in one piece
Ability to transfer exudate to secondary dressing
Ability to support a clean wound bed
Overall impression of dressing
Average wear time of the dressing?
1-2 Days 3-5 Days 5 Days of more
Main reason for dressing changes?
Enter your answer
Were the clinical objectives of using the product met?
Enter your answer
What advantages do you think Exufiber/Exufiber Ag+ has over previously used dressings?
Enter your answer
Would you use Exufiber/Exufiber Ag+ dressings again?
Yes No Maybe
Would you recommend Exufiber/Exufiber Ag+ dressings to other clinicians
Yes No Unsure
Wound types (select all that apply)
Leg ulcers Foot Ulcer Abrasion Skin Tear Blister Traumatic wound Surgical wound Burns Pressure Ulcers
Wound locations
Enter your answer
Use of other interventions such as compression/off-loading (please specify)
Enter your answer
Please list the name(s) of other dressings used
Enter your answer
Clinical reason for using the product
Enter your answer
Clinical reasons for choosing dressing regime
Enter your answer
Size of dressing used
Enter your answer
Please comment on the performance of Exufiber/Exufiber Ag+
Very Good
Good
Adequate
Poor
Ease of handling
Ease/speed of application/use
Consistency of product
Ability to be repositioned during application
Conformability
Patient comfort during wear
Ability to absorb exudate
Ability to retain exudate
Performance when used under compression
Ability to maintain integrity during wear time and on removal
Ease/speed of removal
Ability to be removed in one piece
Ability to transfer exudate to secondary dressing
Ability to support a clean wound bed
Overall impression of dressing
Average wear time of the dressing?
1-2 Days 3-5 Days 5 Days of more
Main reason for dressing changes?
Enter your answer
Were the clinical objectives of using the product met?
Enter your answer
What advantages do you think Exufiber/Exufiber Ag+ has over previously used dressings?
Enter your answer
Would you use Exufiber/Exufiber Ag+ dressings again?
Yes No Maybe
Would you recommend Exufiber/Exufiber Ag+ dressings to other clinicians
Yes No Unsure
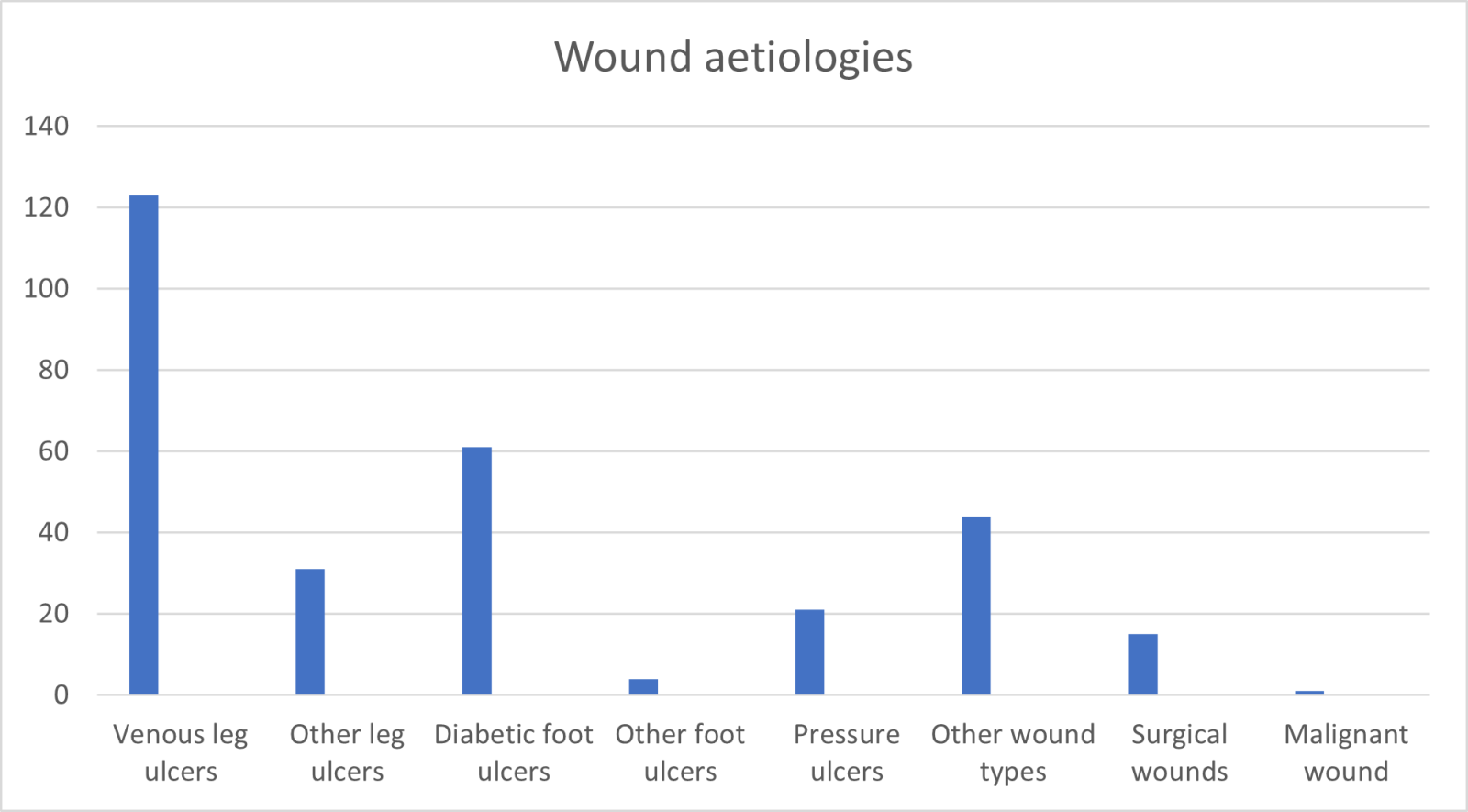
Figure 4. Wound aetiologies
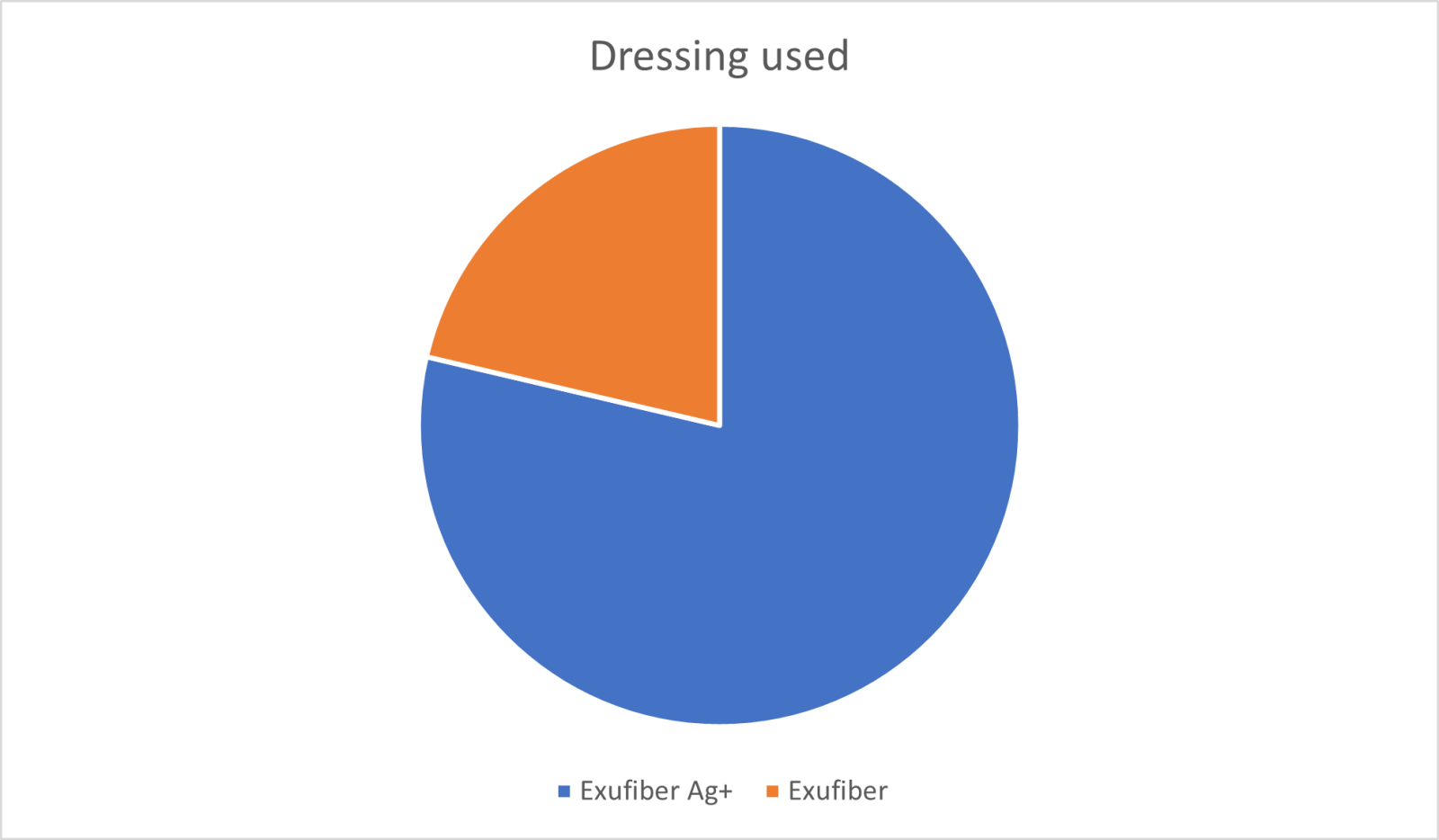
Figure 5. Dressings used
Exufiber Ag+
Of the 236 responses using Exufiber Ag+:
- 99% rated the dressings’ ability to maintain its integrity during wear and on removal as good or very good. This reflects the make up of the dressing, with more tightly packed fibres and the dressing having a high wet strength, allowing one piece removal from the wound
- 94% rated the dressings’ ability to support a clean wound bed as good or very good. As mentioned previously, the Exufiber range forms a soft conformable gel which provides a moist wound healing environment, supporting autolytic debridement and leading to a clean wound bed
- 94% rated the dressings’ ability to transfer fluid to the secondary dressing as good or very good. This feature also relates to the tightly packed fibres of the product helping to transfer fluid from the wound bed to the secondary dressing, even when the dressing is full of fluid, this can help to prevent the pooling of fluid in the wound bed
- 97% rated their overall impression of the dressing as good or very good
- 95% of customers reported the dressing as very good or good in exudate retention under compression. This is a key requirement for products which are used under compression therapy and essential to prevent wound exudate from leaking back onto the wound bed
- 97% would consider using it on other patients. Some clinicians used the product on more than one patient and may have already been using the product
- 99.5% would recommend it to colleagues.
- The product was easy to remove without leaving residue
- Higher cleaning power of the wound bed
- No maceration and better integrity than other products
- Longer stay in wound bed and easy to remove when compared with their normal gelling fibre product
- Transfers exudate well into the secondary dressing and prevents skin maceration
- Exufiber retained exudate and kept it away from the wound bed even under compression
- Good exudate management and excellent under compression bandage
- More absorbing capacity and better debridement than the normal gelling fibre products in use
- Effectively cleans the wound bed.
Exufiber
Of the 64 responses using standard Exufiber, clinician comments were similar to those who used Exufiber Ag+:
- 97% of clinicians rated the dressings’ ability to maintain its integrity during wear and on removal as good or very good
- 96% rated the dressings’ ability to perform under compression therapy as good or very good
- 85% rated the dressings’ ability to transfer fluid to the secondary dressing as good or very good
- 91% rated the dressing good or very good for retention of wound fluid under compression therapy
- 92% rated their overall impression of the dressing as good or very good
- 97% would consider using it on other patients
- 91% would recommend it to colleagues.
- Promotes autolytic debridement. High management of exudate, avoiding the maceration of perilesional (periwound) edges and skin
- Promotes granulation tissue and is removed in one piece
- Daily dressings with another gelling fibre product reduced to 3 times per week with Exufiber
- Good retention capacity compared with product used before
- Better cleaning capacity and debridement
- Benefits of Exufiber over previous product: stayed together better, easier to remove, better exudate absorption.
Discussion
The majority of the wounds reported in the survey were venous leg ulcers which would suggest that, as expected, venous leg ulcers are associated with an increase in exudate volume and a requirement for absorbent dressings, as well as compression therapy (Guest et al, 2018). Both Exufiber and Exufiber Ag+ demonstrated the ability to retain exudate in the dressing, therefore, preventing exudate from leaking out of the dressing and onto the wound bed and/or surrounding skin. 91% in the Exufiber group stated the dressing was very good or good in this aspect for all wound types.
The second most common group were patients with diabetic foot ulceration. Patients with foot ulcers related to diabetes are at higher risk of infection and when infection occurs this can have significant impact on patient morbidity. The majority of patients with foot ulcers in the study were in the Exufiber Ag+ group, indicating the presence of, or the increased risk of infection.
The results of the survey were overall very positive, with many clinicians reporting good or very good experiences with both the Exufiber Ag+ and Exufiber dressings respectively. It is important that wound dressings are able to effectively manage wound exudate in order to reduce the risks of maceration of the periwound skin and also to help reduce the risk of infection (Moore and Strapp, 2015). It is also important for gelling fibre dressings to be removed in one piece thereby preventing pieces of the dressing remaining in the wound bed on removal. This aspect was very positively reported in the survey for both dressings with 99% and 97% of clinicians reporting positively on the dressing integrity on removal. Gelling fibre dressings should support autolytic debridement by forming a soft moist gel on the wound surface that allows debridement to take place between dressing changes. 94% of the Exufiber Ag+ group and 89% of the Exufiber group reported positively on the ability of the dressing to support a clean wound bed.
Conclusion
Gelling fibre dressings are commonly used to manage wounds where exudate volume has the potential to cause delayed healing. This new gelling fibre product range not only helps to manage exudate effectively by absorption and retention but also by enabling the transfer of exudate to a secondary dressing, therefore avoiding the pooling of exudate in the wound bed and reducing the risk of maceration and supporting a clean wound bed.
Limitations
This study is a non-comparative, non-scientific report on the experience of 300 clinicians indicating their real world experience when using Exufiber and Exufiber Ag+. There was no randomisation used in the study and opinions are those of the clinicians using the products.
Acknowledgements
Thanks to Paolo Alves, for providing images, Professor Doutor Paulo Jorge Pereira Alves, Universidade Católica Portuguesa, Instituto Ciências da Saúde and Melanie Williscroft and Marie Dubois from the Mölnlycke marketing department for supporting this project and providing help with the survey.
References
Gibson D, Cullen B, Legerstee R, et al (2009) MMPs Made Easy. Wounds International, London. Available online: http://www.woundsinternational.com
Guest JF, Ayoub N, McIlwraith T, et al (2016) Health economic burden that different wound types impose on the UK’s National Health Service. Int Wound J 14(2): 322-330
Guest JF, Fuller GW, Vowden P (2018) Venous leg ulcer management in clinical practice in the UK: costs and outcomes. Int Wound J 15(1): 29-37
Lustig A, Gefen A (2022) The performance of gelling fibre wound dressings under clinically relevant robotic laboratory tests. Int Wound J 19(Suppl. 1): 3–21
Moore Z, Strapp H (2015) Managing the problem of excess exudate. Br J Nurs 24(15): S12-17
Guest JF, Ayoub N, McIlwraith T, et al (2016) Health economic burden that different wound types impose on the UK’s National Health Service. Int Wound J 14(2): 322-330
Guest JF, Fuller GW, Vowden P (2018) Venous leg ulcer management in clinical practice in the UK: costs and outcomes. Int Wound J 15(1): 29-37
Lustig A, Gefen A (2022) The performance of gelling fibre wound dressings under clinically relevant robotic laboratory tests. Int Wound J 19(Suppl. 1): 3–21
Moore Z, Strapp H (2015) Managing the problem of excess exudate. Br J Nurs 24(15): S12-17

