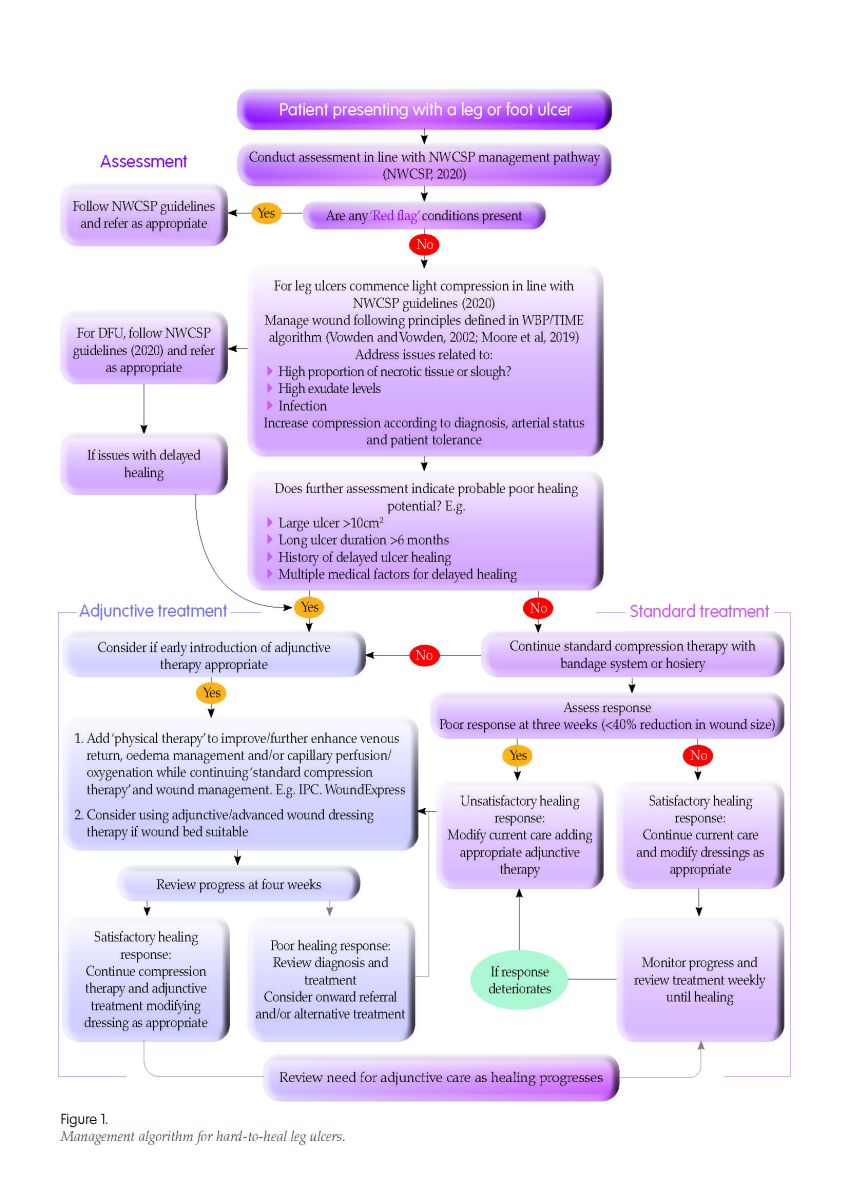
References
Atkins L, Tansley J, Stephenson J (2018) Diabetic foot ulceration: the impact of diabetes. Wounds UK 14(1): 33–9
Bender C, Cichosz SL, Pape-Haugaard L, Hartun Jensen M, Bermark S, Laursen AC, et al (2020) Assessment of simple bedside wound characteristics for a prediction model for diabetic foot ulcer outcomes. J Diabetes Sci Technol 2020: 1932296820942307
Bergant Suhodolcan A, Luzar B, Kecelj Leskovec N (2021) Matrix metalloproteinase (MMP)-1 and MMP- 2, but not COX-2 serve as additional predictors for chronic venous ulcer healing. Wound Repair Regen 29(5): 725–31
Bosanquet DC, Sanders AJ, Ruge F, Lane J, Morris CA, Jiang WG, et al (2019) Development and validation of a gene expression test to identify hard-to-heal chronic venous leg ulcers. Br J Surg 106(8): 1035–42
Bui UT, Edwards H, Finlayson K (2018) Identifying risk factors associated with infection in patients with chronic leg ulcers. Int Wound J 15(2): 283–90
Bull RH, Staines KL, Collarte AJ, Bain DS, Ivins NM, Harding KG (2021) Measuring progress to healing: A challenge and an opportunity. Int Wound J. Available online: https://onlinelibrary.wiley.com/doi/pdf/10.1111/iwj.13669
Canedo-Dorantes L, Canedo-Ayala M (2019) Skin acute wound healing: a comprehensive review. Int J Inflam 2019: 3706315
Chen SM, Ward SI, Olutoye OO, Diegelmann RF, Kelman CI (1997) Ability of chronic wound fluids to degrade peptide growth factors is associated with increased levels of elastase activity and diminished levels of proteinase inhibitors. Wound Repair Regen 5(1): 23–32
Dissemond J, Augustin M, Dietlein M, Faust U, Keuthage W, Lobmann R, et al (2020) Efficacy of MMP-inhibiting wound dressings in the treatment of chronic wounds: a systematic review. J Wound Care 29(2): 102–18
Edwards HE, Parker CN, Miller C, Gibb M, Kapp S, Ogrin R, et al (2018) Predicting delayed healing: The diagnostic accuracy of a venous leg ulcer risk assessment tool. Int Wound J 15(2): 258–65
Flanagan M (2003a) Improving accuracy of wound measurement in clinical practice. Ostomy Wound Manage 49(10): 28–40
Flanagan M (2003b) Wound measurement: can it help us to monitor progression to healing? J Wound Care 12(5): 189–94
Fletcher J, Dowsett C, Reader SH, Ousey K, Pagnamenta F, Vernon T, et al (2020) Best Practice Statement: Management of lower limb skin tears. Wounds UK, London
Franks PJ, Barker J, Collier M, Gethin G, Haesler E, Jawien A, et al (2016) Management of Patients With Venous Leg Ulcers: Challenges and Current Best Practice. J Wound Care 25 Suppl 6: S1–S67
Gelfand JM, Hoffstad O, Margolis DJ (2002) Surrogate endpoints for the treatment of venous leg ulcers. J Invest Dermatol 119(6): 1420–5
Gethin G (2006) The importance of continuous wound measuring. Wounds UK 2(2): 60–7
Gilman T (2004) Wound outcomes: the utility of surface measures. Int J Low Extrem Wounds 3(3): 125–32
Guest JF, Ayoub N, McIlwraith T, Uchegbu I, Gerrish A, Weidlich D, et al (2015) Health economic burden that wounds impose on the national health service in the UK. BMJ Open 5(12): e009283
Guest JF, Ayoub N, Mcilwraith T, Uchegbu I, Gerrish A, Weidlich D, et al (2017) Health economic burden that different wound types impose on the UK’s National Health Service. Int Wound J 14(2): 322–30
Guest JF, Fuller G, Vowden P (2018a) Venous leg ulcer management in clinical practice in the UK: costs and outcomes. Int Wound J 15: 29–37
Guest JF, Fuller GW, Vowden P, Vowden K (2018b) Cohort study evaluating pressure ulcer management in clinical practice in the UK following initial presentation in the community: costs and outcomes. BMJ Open 8: e021769
Guest JF, Fuller GW, Vowden P (2020) Cohort study evaluating the burden of wounds to the UK’s National Health Service in 2017/2018: update from 2012/2013. BMJ Open 10(12): e045253
Harding KG, Morris HL, Patel GK (2002) Science, medicine and the future: healing chronic wounds. Br Med J 324(7330): 160–3
Ho TK, Leigh RD, Tsui J (2013) Diabetic foot disease and oedema. Br J Diabetes Vasc Dis 13(1): 45–50
Horn SD, Barrett RS, Fife CE, Thomson B (2015) A predictive model for pressure ulcer outcome: the Wound Healing Index. Adv Skin Wound Care 28(12): 560–72; quiz 73–4
Itoh M, Montemayor JS, Jr, Matsumoto E, Eason A, Lee MH, Folk FS (1991) Accelerated wound healing of pressure ulcers by pulsed high peak power electromagnetic energy (Diapulse). Decubitus 4(1): 24–5, 9–34
iWoundnews (2019) National Wound Care Strategy aiming for ‘excellence’ across lower limb and surgical work streams.
Kramer JD, Kearney M (2000) Patient, wound, and treatment characteristics associated with healing in pressure ulcers. Adv Skin Wound Care 13(1): 17–24
Ladwig GP, Robson MC, Liu R, Kuhn MA, Muir DF, Schultz GS (2002) Ratios ofactivated matrix metalloproteinase-9 to tissue inhibitor of matrix metalloproteinase-1 in wound fluids are inversely correlated with healing of pressure ulcers. Wound Repair Regen 10(1): 26–37
Lauer G, Sollberg S, Cole M, Flamme I, Sturzebecher J, Mann K, et al (2000) Expression and proteolysis of vascular endothelial growth factor is increased in chronic wounds. J Invest Dermatol 115(1): 12–8
Lazaro JL, Izzo V, Meaume S, Davies AH, Lobmann R, Uccioli L (2016) Elevated levels of matrix metalloproteinases and chronic wound healing: an updated review of clinical evidence. J Wound Care 25(5): 277–87
LeBlanc K, Baranoski S, International Skin Tear Advisory Panel (2014) Skin tears: best practices for care and prevention. Nursing. 44(5): 36–46; quiz 8
LeBlanc K, Campbell K, Beeckman D, Dunk AM, Harley C, Hevia H, et al(2018) Best practice recommendations for the prevention and management of skin tears in aged skin. Wounds Innternational, London. Available online: www.woundsinternational.com
Medina A, Scott PG, Ghahary A, Tredget EE (2005) Pathophysiology of chronic non- healing wounds. J Burn Care Rehabil 26(4): 306–19
Milne J, Searle R, Styche T (2020) The characteristics and impact of hard-to-heal wounds: results of a standardised survey. J Wound Care 29(5): 282–8
Moffatt C, Vowden P (2008) Hard-to-heal wounds: a holistic approach. In: EWMA Position Document: Hard-to-heal wounds: a holistic approach. MEP Ltd, London: 1–7
Moore Z, Dowsett C, Smith G, Atkin L, Bain M, Lahmann NA, et al (2019) TIME CDST: an updated tool to address the current challenges in wound care. J Wound Care 28(3): 154–61
National Wound Care Strategy Programme (2020) Recommendations for Lower Limb Ulcers.
Nelson EA, Hillman A, Thomas K (2014) Intermittent pneumatic compression for treating venous leg ulcers. Cochrane Database Syst Rev (5): CD001899
Oien RF, Forssell H, Ragnarson Tennvall G (2016) Cost consequences due to reduced ulcer healing times — analyses based on the Swedish Registry of Ulcer Treatment. Int Wound J 13(5): 957–62
Parker CN, Finlayson KJ, Shuter P, Edwards HE (2015) Risk factors for delayed healing in venous leg ulcers: a review of the literature. Int J Clin Pract 69(9): 967–77
Parker CN, Finlayson KJ, Edwards HE (2017) Predicting the likelihood of delayed venous leg ulcer healing and recurrence: development and reliability testing of risk assessment tools. Ostomy Wound Manage. 63(10): 16–33
Phillips TJ, Machado F, Trout R, Porter J, Olin J, Falanga V (2000) Prognostic indicators in venous ulcers. J Am Acad Dermatol 43(4): 627–30
Prince S, Dodds SR (2006) Use of ulcer size and initial response to treatment to predict the healing time of leg ulcers. J Wound Care 15(7): 299–303
Raffetto JD (2016) Pathophysiology of wound healing and alterations in venous leg ulcers-review. Phlebology 31(1 Suppl): 56–62
Raffetto JD, Ligi D, Maniscalco R, Khalil RA, Mannello F (2020) Why venous leg ulcers have difficulty healing: overview on pathophysiology, clinical consequences, and treatment. J Clin Med 10(1): 29
Shi C, Dumville JC, Cullum N, Connaughton E, Norman G (2021) Compression bandages or stockings versus no compression for treating venous leg ulcers. Cochrane Database Syst Rev 7: CD013397
Stacey MC (2020) Biomarker directed chronic wound therapy — a new treatment paradigm. J Tissue Viability 29(3): 180–3
Steed DL, Hill DP, Woodske ME, Payne WG, Robson MC (2006) Wound-healing trajectories as outcome measures of venous stasis ulcer treatment. Int Wound J 3(1): 40–7
Tardaguila-Garcia A, Garcia-Morales E, Garcia-Alamino JM, Alvaro-Afonso FJ, Molines-Barroso RJ, Lazaro-Martinez JL (2019) Metalloproteinases in chronic and acute wounds: A systematic review and meta-analysis. Wound Repair Regen 27(4): 415–20
Tarlton JF, Bailey AJ, Crawford E, Jones D, Moore K, Harding KD (1999) Prognostic value of markers of collagen remodeling in venous ulcers. Wound Repair Regen 7(5): 347–55
Tay WL, Lo ZJ, Hong Q, Yong E, Chandrasekar S, Tan GWL (2019) Toe pressure in predicting diabetic foot ulcer healing: a systematic review and meta- analysis. Ann Vasc Surg 60: 371–8
Trengove NJ, Stacey MC, MacAuley S, Bennett N, Gibson J, Burslem F, et al (1999) Analysis of the acute and chronic wound environments: the role of proteases and their inhibitors. Wound Repair Regen 7(6): 442–52
Troxler M, Vowden K, Vowden P (2006) Integrating adjunctive therapy into practice: the importance of recognising ‘hard-to- heal’ wounds.
van Rijswijk L (1993) Full-thickness leg ulcers: patient demographics and predictors of healing. Multi-Center Leg Ulcer Study Group. J Fam Pract 36(6): 625–32
Vowden P, Vowden K (2002) Wound Bed Preparation (WBP). World Wide Wounds.
Vowden P, Vowden K (2016) The economic impact of hard-to-heal wounds: promoting practice change to address passivity in wound management. Wounds Int 7(2): 10–5
Westby MJ, Dumville JC, Stubbs N, Norman G, Wong JK, Cullum N, et al (2018) Protease activity as a prognostic factor for wound healing in venous leg ulcers. Cochrane Database Syst Rev 9: CD012841
Wilkinson HN, Hardman MJ (2020) Wound healing: cellular mechanisms and pathological outcomes. Open Biol 10(9): 200223
Xu Y, Sun J, Carter RR, Bogie KM (2014) Personalized prediction of chronic wound healing: an exponential mixed effects model using stereophotogrammetric measurement. J Tissue Viability 23(2): 48–59
Young T, Chadwick P, Fletcher J, King B, Schofield A, Staines K, et al (2021) The Benefits Of Intermittent Pneumatic Compression And How To Use WoundexpressTM In Practice. Available online: www.wounds-uk.com.